Training surgeons to manage stress, emotions
By Ramtin Hakimjavadi, BMSc Candidate
‘Amygdala hijacking’ – when stressful situations cause your executive function to falter and emotions overpower your better judgement. It’s an emotional response that often results in a sudden drop in performance.
 For surgeons, the phenomenon can have dire consequences.
For surgeons, the phenomenon can have dire consequences.
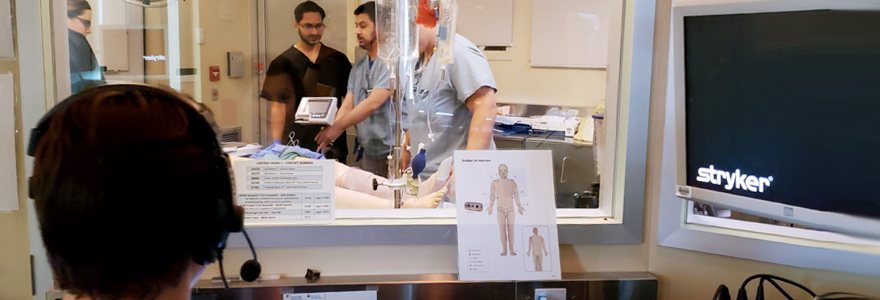
A simulation program at Schulich Medicine & Dentistry is helping train surgical residents to effectively manage high-stress, emotional scenarios. Developed by Dr. Robert Leeper, MD’07, Assistant Professor with the Department of Surgery, the program uses team-based simulation scenarios to train general surgery residents in trauma resuscitation.
First-year resident Dr. Nicholas Mitrou, MD’19, is an active participant and part of a research team looking at the program’s learning outcomes. "At the start of the simulation scenario, we have no clue what to expect,” he said. “All we know is that it will have something to do with trauma resuscitation.”
Drs. Leeper and Mitrou recently co-authored a study evaluating the technical and non-technical skills developed during the course of this novel program.
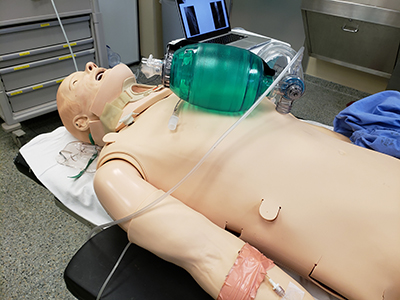
Simulation provides plenty of advantages in medical training: there is no risk to patients, rare scenarios can be staged and errors can be allowed to unfold, enabling learners to practice dealing with potentially disastrous situations. Importantly, simulating real-life clinical scenarios exposes surgical residents to the suite of emotions they will encounter once they are in the field.
The longitudinal application of this simulation program repeatedly exposes residents to high-stress scenarios. During the course of a year, their minds become conditioned to what they will inevitably face as surgeons. “This allows for stress inoculation, giving you a vaccine against stress,” explained Dr. Leeper.
“It creates a more bulletproof mind so that when you are in the field and the psychological bullets are flying, they bounce off you.”
 The program includes a unique debriefing phase, an essential component of the curriculum that allows learners to reflect on the scenarios they encounter. “Simulation is the substrate whereas debriefing is the art-form. The debriefing is really what makes the knowledge come through and last,” said Dr. Leeper.
The program includes a unique debriefing phase, an essential component of the curriculum that allows learners to reflect on the scenarios they encounter. “Simulation is the substrate whereas debriefing is the art-form. The debriefing is really what makes the knowledge come through and last,” said Dr. Leeper.
Each resident is also given personalized narrated video feedback. This way, they can digest feedback at their own pace, allowing for delayed and distributed reflection. The long-term exposure to trauma simulations with a prolonged debriefing phase creates an environment for continuous learning with ample time for introspection.
The program takes a novel approach to quality improvement, introducing a positive competitive environment that helps surgical residents thrive. Leveraging the innate competitiveness of surgeons, the program fosters positive change in individual and team performance.
To implement this team-based competition requires careful orchestration. "We do a lot to make it psychologically safe," explained Dr. Leeper. Teams receive anonymized ordinal rankings after each session. They are given their own rank compared to other teams, but the standings of the other teams are not disclosed. This anonymity breeds psychological safety and encourages teams to collectively perform better.
 Drs. Leeper and Mitrou found that in the trauma simulation curriculum there was a strong positive correlation between the development of technical and non-technical skills. Learning more about the directionality in this relationship could reveal key insights about the benefits of simulation training.
Drs. Leeper and Mitrou found that in the trauma simulation curriculum there was a strong positive correlation between the development of technical and non-technical skills. Learning more about the directionality in this relationship could reveal key insights about the benefits of simulation training.
"Our hope is that improvements in teamwork drive improvements in technical performance. But that is still an open question," said Dr. Mitrou. With many more simulations to come as part of his residency journey, he will continue to generate data for future studies.