Code Blue
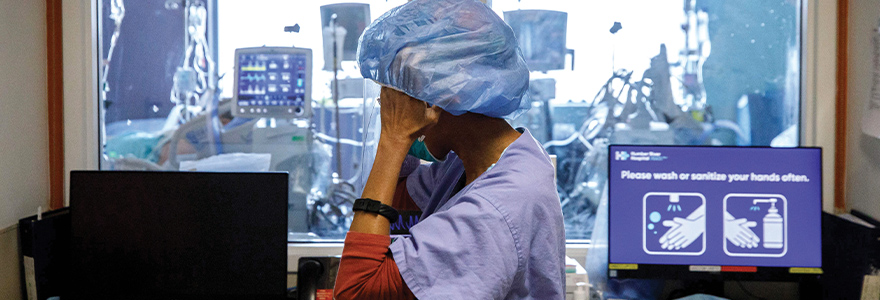 A health-care worker dons a bouffant cap at Humber River Hospital’s Intensive Care Unit, in Toronto, Ontario.
A health-care worker dons a bouffant cap at Humber River Hospital’s Intensive Care Unit, in Toronto, Ontario. Photo by Cole Burston via Getty Images.
For many Canadians, the pandemic is over – but not for our health-care workers. How have they fared through the pandemic? And are we doing enough to take care of those who took care of us?
Amanda looked at the face that stared back at her from the bathroom mirror – chafe marks from the mask, lines around the mouth, sleepless eyes rimmed with black. Who was that person? “I’ve got to get out of here,” thought the 30-year-old family physician, now pulled into the emergency room by the demands of the pandemic, the rising death counts and the shortage of physicians. Beyond the bathroom came the sounds of doctors and nurses yelling, patients calling for help, the beeping, the buzzing, the crying. And piercing through it all, the sound of a monitor emitting that flatline tone that indicated another death. Another reason to give up, quit, hide, or worse. Amanda shoved shaking hands into the pockets of her scrubs, and shouldered the door open, heading back into battle.
In May 2023, the World Health Organization declared “with great hope” the end of COVID-19 as a public health emergency. Yet physicians, nurses, and other health professionals are still suffering the effects of three years on the frontlines, including drug abuse, suicides, and mental health issues.
And while fictional, the above account captures some of the pressures faced by health-care workers as a result of the pandemic.
Schulich Medicine & Dentistry researchers have uncovered some alarming details about how widespread the problem is. Dr. Don Richardson’s work highlights the problem. Richardson is a professor in the Department of Psychiatry and scientific director of the MacDonald Franklin OSI Research Centre at St. Joseph’s Health Care London.
His 18-month study reveals an alarming mental health crisis among health-care workers during the pandemic: 39 per cent suffered from probable post-traumatic stress disorder (PTSD), 52 per cent battled major depressive disorder, while 19 per cent experienced suicidal thoughts, emphasizing the urgent need for support. Additionally, 44 per cent considered leaving their positions due to moral distress, highlighting the profound impact of the pandemic on health-care workers.
THE TRUTH ABOUT
PHYSICIAN HEALTH
39%
suffer from probable PTSD
52%
suffer from major depressive disorder
44%
were considering leaving their
position due to moral distress
19%
experienced suicidal thoughts
“Health-care workers faced excruciating moral dilemmas,” explained Richardson. “On one end, it could involve being directed to reduce patient treatment frequency, while on the other, they had to make heart-wrenching choices, such as allocating respirators or denying dying patients’ loved ones access to their bedside. These decisions also sparked personal fears about falling ill and being in the ICU without the support of their loved ones.”

“Physicians are people and they get sick, too. But no physician wants to come in the front doors of their emergency room.”
—Dr. Andrea Lum
‘Physicians are people and they get sick, too’
When two prominent Alberta surgeons died by suicide last year, it was a wake-up call that some physicians were in critical condition, but afraid to admit it.
“Physicians are people and they get sick, too,” said Dr. Andrea Lum, vice dean, Clinical Faculty Affairs, at Schulich Medicine & Dentistry. “But no physician wants to come in the front doors of their emergency room.”
With that in mind, the School’s much-emulated Peers for Peers program is leading the charge to approach physician mental health in a new way. While organizations such as the Ontario Medical Association offer specific mental health support for physicians, Schulich Medicine & Dentistry provides the only comprehensive peer-based program in the country specifically for clinical faculty.
The Peers for Peers training program is now being used in coastal British Columbia, at the Northern Ontario School of Medicine, and in Saskatchewan. Plus, health-care authorities from as far away as India have expressed interest.
Peers for Peers – the brainchild of Lum – was inspired by a similar empathetic listening program created for airline pilots. Despite having the same access to employee assistance programs as everyone else at the airline, pilots just weren’t reaching out because they felt only other pilots could understand their stress.
“Pilots are not unlike physicians,” said Dr. Laura Foxcroft, assistant dean of Faculty Well-Being, who was hired in October 2022 to run the program. “They’re highly skilled in looking after people and mostly things go well. But when they don’t, it’s devastating.”

“Health-care workers faced excruciating moral dilemmas... They had to make heartwrenching choices, such as allocating respirators or denying dying patients’ loved ones access to their bedside.”
—Dr. Don Richardson
Shifting the culture
Launched at the start of the pandemic, Peers for Peers has now trained more than 55 faculty members in the skill of physician peer support, which is rooted in empathetic listening.
Lum and Foxcroft feel Peers for Peers has shifted the culture around physicians seeking help, making it more acceptable to reach out, despite concerns of confidentiality, stigma, and professional identities. While they don’t track numbers, the doctors said in the three years since it has been operating, approximately one-third of clinical faculty have used the program.
“We found eight out of 10 times a physician talked to a peer, that was enough. That gave them the feeling somebody understood the space they were in and it gave them the energy to go on,” said Foxcroft.
In the two out of 10 interactions where peer support wasn’t enough, peer supporters provided resources to “psychologically safe” mental health resources that allowed them to get help.

“We found eight out of 10 times a physician talked to a peer, that was enough. That gave them the feeling somebody understood the space they were in and it gave them the energy to go on.”
—Dr. Laura Foxcroft
What comes next?
Peers for Peers is now evolving to include three new training modules that will be ready this fall. The first involves something called ‘Check you, check two,’ whereby physicians are trained to rate their own mental health at the beginning of the day, and if it’s good, check in with two colleagues.
“Most physicians will say, ‘Yeah, yeah, I’m fine,’” admitted Foxcroft. “But we find that two or three weeks later, it opens the door to physicians reaching out to their peer supporter to say, ‘I’m actually not OK. I need resources for this, this and this.’”
The other new modules will focus on two important topics: Intimate Partner Violence amongst physicians, and providing trauma-informed care to physicians. These two new modules are being created by Dr. Susan McNair, a faculty member with expertise in this area.
Foxcroft is one of many who know what the current environment feels like: “I am an emergency medicine physician. When I go in for my shift tonight, the waits will be long and the first patient I see is often angry because they have waited so long. Physician well-being is contingent on working in a system that has the resources available in a timely manner to provide the care I was trained to provide.”
In a groundbreaking move, Richardson and Dr. Anthony Nazarov at the MacDonald Franklin OSI Research Centre launched the Public Health Agency of Canada funded Healthcare Worker WellBeing Initiative in June 2022. Their initial goal was to adapt the Road to Mental Readiness program originally designed for the Canadian military, focusing on addressing PTSD and improving mental health literacy.
After extensive feedback from physicians and health-care workers, it became clear that conventional mental health modules, such as yoga and mindfulness, were not what health-care workers needed amidst their already stressful work life. The prevailing message was, ‘We need support in an environment not conducive to mental health right now.’
This feedback prompted Richardson’s team to shift the focus towards a comprehensive framework – the Revel Method. This innovative approach empowers health-care workers through engaging strategies, tackling workplace well-being, burnout, and demoralization, while transforming the work environment for these dedicated professionals.
In the meantime, health-care workers continue to face the demands and experience the impact of a system that doesn’t provide the necessary support they need to thrive. But with programs like Peers for Peers and the Revel Method, Schulich Medicine & Dentistry researchers are paving the way for a better future.
LESSONS FROM THE PANDEMIC
If COVID-19 has taught us anything about the health-care system, it’s that focusing solely on the mental resilience of individual physicians, nurses and others is a mistake.
“It can detract from the underlying problem,” said Dr. Ruth Lanius, professor of Psychiatry and Harris-Woodman Chair in Mind-Body Medicine. “We’re in desperate need of making significant changes to our health-care system.”
Lanius, along with colleagues at McMaster University, developed five recommendations for retaining skilled health-care workers.
“If these important issues are not addressed, we will likely face an ongoing exodus of skilled health-care workers,” she said.
Tips for maintaining healthy health-care workers
- Support healthcare provider mental health and well-being
- Use concise and transparent communication when distributing updates or changes to policy
- Explain the rationale for all decisions and offer opportunity for input
- Provide organizational support dedicated to fostering strong teams in the workplace
- Encourage professional autonomy and respect at all levels of the organization








