Education
Contact Us
Program Director, Dr. Rachel Reardon
Vanessa Cullen, Program Administrator
Email: Program.Admin@sjhc.london.on.ca
Postgraduate

Schulich School of Medicine & Dentistry, Western University has a well-respected residency program with a consistent history of graduating residents who are well prepared for the Royal College and EMG exams, and who are desirable candidates for competitive fellowships and academic positions.
The program has an excellent resident to faculty ratio with an engaged, education focused faculty.
Interdisciplinary collaborative care between Physiatry and other specialties (Orthopedics, Plastics, Neurology, etc) provides unique educational experiences for our residents.
We are part of a large, academic, medical community with a full complement of medical services to allow for a comprehensive residency education without need for travel to other centres.
The City of London provides an excellent setting for resident education, with a combination of beautiful parks and bike trails, excellent cost of living, and a vibrant community with world class concerts, festivals, and dining.
Further details of the Program can also be found on the CANPREPP website.
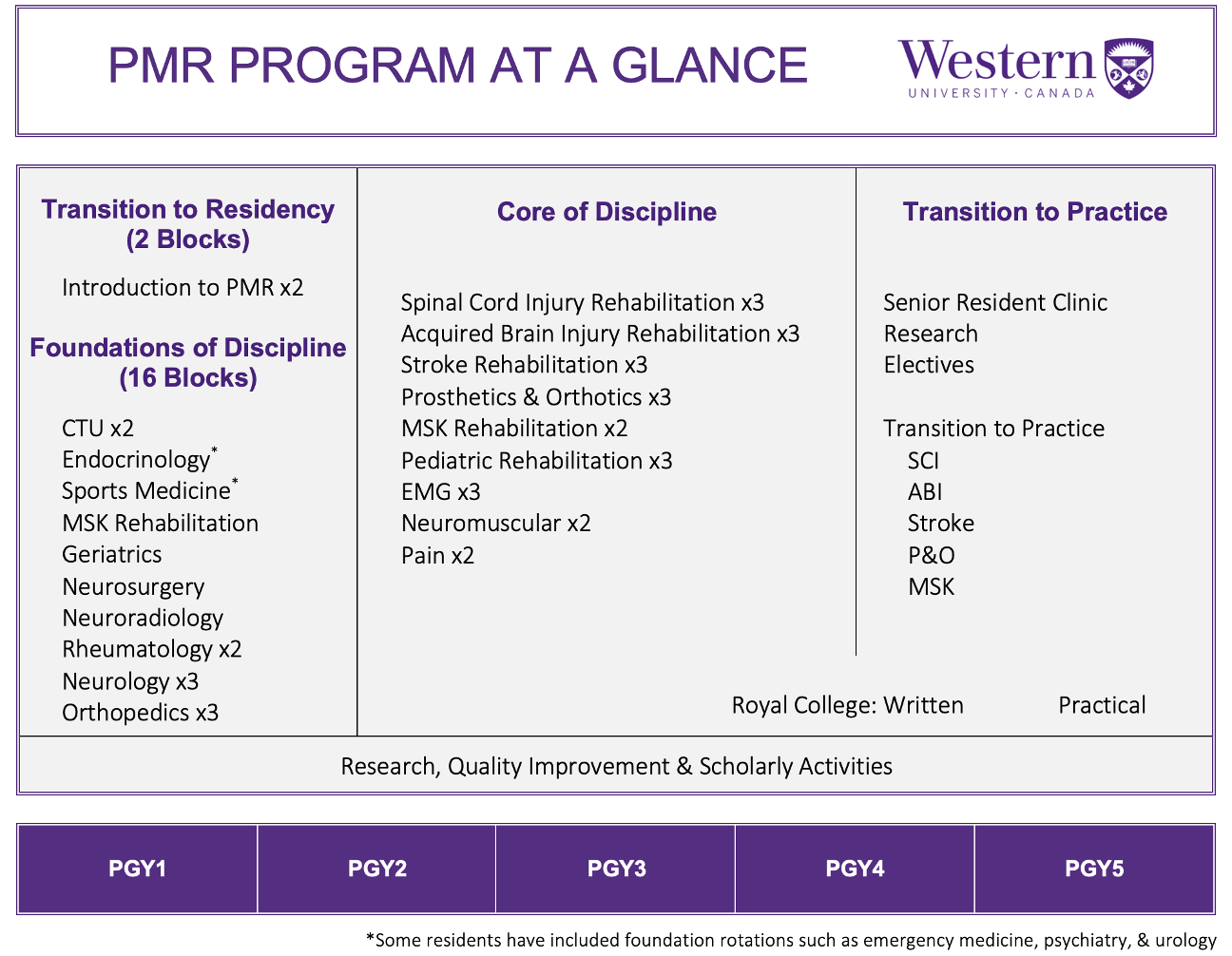
Education
The Physical Medicine & Rehabilitation program at the Schulich School of Medicine & Dentistry, Western University has a faculty dedicated to clinical and didactic medical education.
The residency program has formal Academic Half-Days on Monday mornings, which are protected learning times where residents are provided education covering all aspects of the Royal College Learning Objectives.
Academic Half-days also include additional learning experiences including Journal Club/Evidence-Based Medicine Rounds, Grand Rounds, Hand and Upper Limb Surgical/PM&R Rounds, and Quality Assurance and Patient Safety Rounds.
Additional formal learning opportunities occur one-on-one with faculty during each trainee's CORE physiatry rotations. These are a mix of resident tailored teaching sessions, and clinical hands-on learning.
The residents also have additional learning experiences every year including our Summer Cadaver-based Anatomy sessions, Ultrasound guided injection learning sessions with our Sport Medicine and Pain fellows, and additional opportunities to attend City-Wide Department of Medicine, Neurology and Neuromuscular rounds (amongst others).
In addition, we provide residents with regular practice written exams and OSCEs (Standard OSCE and Teaching OSCE) including opportunity to engage in Inter-City (ie. Tri-City) practice exams with the University of Toronto and McMaster.
Residents are responsible for participating in the teaching of medical students and their fellow residents. Friday mornings are set aside for resident-run teaching sessions for all those currently on CORE physiatry rotations at Parkwood Institute.
Training Sites
Parkwood Institute
This is the site of most of the core training in Physical Medicine & Rehabilitation including EMG, MSK, Stroke rehab, ABI, SCI, Prosthetics and Orthotics and other. The Geriatrics and Mental Health teams are also located here.
St. Joseph's Health Care London
This is the site for the Hand and Upper Limb Clinic and Multidisciplinary Chronic Pain clinic along with additional sub-speciality medicine clinics such as Rheumatology, and Endocrinology.
Fowler Kennedy Sport Medicine Clinic - 3M Centre Western University
This is the site of our Sports Medicine rotation.
London Health Science Centre
The majority of Foundations of Discipline rotations including Internal Medicine and Surgical Services occur between the two LHSC sites – University Hospital and Victoria Hospital.
Children's Hospital at LHSC
This is one of the sites where residents will work during their pediatric rehabilitation rotation, in addition to the Thames Valley Children’s Centre (TVCC), and Parkwood Institute.
Research and Quality Improvement
The Department of PM&R has a group of physicians, and other team members with a strong focus on research and quality improvement.
This includes members of The Gray Centre for Mobility and Activity, a newly formed multi-disciplinary initiative focussed on optimizing health and mobility through the life span.
Please see our Faculty member profile page, and click on Biography for more details of each staff physician’s research interests.
Residents are provided the tools and resources required to complete a Scholarly Project in research AND/OR quality improvement including faculty mentorship, funding, and dedicated time (at least 3 blocks). Formal teaching is provided during Academic Half Day lectures on the foundational knowledge pertaining to Research Methodology, and a formal curriculum (in conjunction with the Department of Medicine) is available for resident’s interested in Quality Improvement.
Additional team members at Parkwood and Western are also available to help guide learners through ethics, statistics and other challenges.
Residents will present an update on their projects each year (Starting in year two (2)) at our PM&R Research Day. Residents will have a role in all aspects of the project from planning, ethics submission, data collection, analysis and manuscription preparation. Projects will be expected to reach a publishable level and residents are encouraged to present their data at the CAPM&R Annual Scientific Meeting or other National and International Conferences. Funding is provided to residents (speak to our residents for details) to travel and present their projects.
Clinical Expectations
On CORE physiatry rotations residents will be delegated responsibilities commensurate with their level of training. They are sometimes joined by more senior resident colleagues (R5) who will have a heightened level of responsibility, acting as a Junior consultant under the supervision of their faculty supervisor.
Inpatient rehabilitation patients are situated at Parkwood Hospital with daily patient care shared between Physiatrists and Hospitalists (ie. Family Medicine Colleagues). This allows for a team approach to medical care and affords Physiatrists and residents opportunities to provide diverse outpatient care at and off-site from Parkwood.
The provision of rehabilitative care is really a team effort, with our Staff and Residents working as part of an integrated team of allied health members and nurses. Residents will participate in inter-disciplinary rounds, and learn one-on-one from their non-MD colleagues.
On-call schedules are prepared monthly by the Lead resident. On-call responsibilities meet PAIRO guidelines. While we acknowledge that being on-call is service oriented, it does additionally provide valuable teaching and learning opportunities. A consultant is always on-call with our residents.
In-Training Evaluations
Our program has been constructed so that adequate exposure will be provided in all major areas of PM&R, sufficient to prepare the resident for the Royal College Fellowship Examination.
Residents are enrolled in a CBME Competence By Design (CBD) program. This means residents will be expected to meet the Entrustable Professional Activity (EPA) requirements for each stage of training. Schulich uses the Elentra platform to collect daily observation forms.
In addition, the Royal College Objectives have been mapped and In-training Evaluation Reports (ITER’s) have been created to cover additional areas not captured by the EPA forms. For example, assessment of each individual resident's performance is done at the mid-point and at the end of each three-block CORE rotation.
The ITER’s, EPA’s, and performance on annual practice exams is collated and reviewed by our Physical Medicine & Rehabilitation Competence Committee on a quarterly basis. This committee made up of appointed faculty members, and an elected resident representative, will provide recommendations to the Program Director regarding whether a resident’s performance is ON TRACK or lagging behind.
In addition, each resident has a formal Program Director (PD)-Resident meeting twice yearly to discuss their progress.
Our program also has a robust Faculty Evaluation program with anonymous resident evaluations being reviewed by the Chair/Chief and discussed with Faculty at their annual performance review.
Holidays
Residents are allowed one week of holiday time during each three-month rotation (additional holidays can be arranged based on application and circumstances). Statutory holidays will be distributed equitably. A five-day holiday period will be arranged over the Christmas period. All holidays must be arranged through the Lead Resident, Program Director, Program Assistant, and the individual consultant on a given service.
Appeal Mechanism
Postgraduate medical trainees whose performance has been judged unsatisfactory by their teachers have the right to appeal. The grounds of an appeal may include medical, compassionate or extenuating circumstances, bias, inaccuracy or unfairness.
The full Appeal Mechanism Policy is available through the Western University Postgraduate Medical Education Office.
PGME Policies
Schulich Medicine PGME Policies, please see the https://www.schulich.uwo.ca/medicine/postgraduate/academic_
Additional Resources can be found here:
https://www.schulich.uwo.ca/medicine/postgraduate/current_learners/index.html
Residency Overview and Royal College Requirements
The Royal College link below provides information by discipline and includes both competencies and training experiences.
Royal College Standards & Accreditation
Transition to Discipline (TTD)
- Initial rotation on Physical Medicine and Rehabilitation ensure new residents are provided an orientation to Parkwood Institute, Western, London and the specialty of Physical Medicine & Rehabilitation.
- Rotation will include inpatient and outpatient duties at Parkwood Institute.
- Goals will include completion of first five EPA's, gaining familiarity with patient care at our centre, exposure to the patient population we serve, and meeting and interacting with our faculty, administrative personnel, residents, and allied health members.
EPAs
- Performing Physiatry-focused histories
- Performing Physiatry-focused physical examinations
- Generating a problem list based on the International Classification of Functioning (ICF) Framework
- Completing clinical documentation
- Providing patient handover
- This portion of residency will provide you the relevant background in general medicine, orthopedics, rheumatology, neurology, and other relevant areas to form the knowledge foundation to provide medical care to our patient populations.
- You will be exposed to patients with a wide range of impairments, activity limitations, and participation restrictions.
- You will be expected to become competent at identifying and managing common emergencies our patients face, while gaining the medical knowledge to provide care pertaining to the wide range of medical co-morbidities that our patients experience.
EPAs
- Assessing and managing patients with non-emergent commonly encountered medical, and surgical issues.
- Identifying, assessing, and providing initial management of patients with emergent and urgent medical issues, and recognizing when to ask for assistance.
- Performing procedures.
Core of Discipline (COD)
- During this part of residency you will gain on-service exposure to all core physiatry areas including Brain Injury, Stroke, Amputee, P+O, Musculoskeletal, Neuromuscular, Cardiac, SCI, Pediatrics, EMG and others.
- You will spend the time required to acquire competency for all core skills required to provide comprehensive management for our patient population.
- This will account for the largest portion of your residency and will prepare you for the Royal College exam.
EPAs
- Providing consultation and developing comprehensive management plans for patients with complex presentations
- Providing ongoing assessment and management for patients with complex presentations
- Identifying, assessing, and managing patients with emergent and urgent medical issues
- Providing consultation and developing management plans for children with common pediatric rehabilitation conditions
- Performing common physiatric procedures
- Selecting and interpreting investigations relevant to Physiatry
- Leading inter-professional meetings.
- Facilitating the learning of others.
Transition of Practice (TTP)
- The final stage of your residency training is focused on consolidating your knowledge, and preparing for your transition to functioning as an independent physiatrist.
- The curriculum will be tailored to each resident's particular career path and goals, and will serve as a way to ensure residents are provided experiences which will make the transition to independent practice as smooth as possible.
- Residents will also be asked to consider their future role as a health advocate for their patients, as well as a self-advocate to ensure they have a plan in place in order to minimize physician burnout.
EPAs
- Managing a physiatric practice.
- Developing a strategy for continuing professional development
Special Assessments
- Planning and completing personalized training experiences aligned with career plans and/or specific learning needs.
- Contributing to the improvement of health care delivery for persons with impairments/disabilities
- Conducting a scholarly project from inception to completion








